Young girl has life-saving gene therapy using world’s most expensive drug at Manchester hospital in a UK first
and live on Freeview channel 276
A Manchester hospital has achieved a major UK medical first after a young girl was given life-saving gene therapy treatment for a deadly disorder using the world’s most expensive drug.
The Royal Manchester Children’s Hospital treated a 20-month old youngster called Teddi with a therapy known by its brand name Libmeldy. This has a list price of £2.8m and even after the NHS obtained a substantial discount for patients in the UK it remains Europe’s most expensive drug.
Advertisement
Hide AdAdvertisement
Hide AdTeddi has metachromatic leukodystrophy (MLD), which causes such severe damage to the nervous system and organs that children with it sadly have a life expectancy of just five to eight years.
Only five sites in Europe offer the treatment - and the prestigious Manchester children’s hospital is the only one in the UK. Sadly, though, the treatment was also a bittersweet moment for Teddi’s family as her older sister also has the genetic disease but was not eligible for Libmeldy.
Why is Teddi’s treatment for MLD with Libmeldy in Manchester so significant?
Teddi, who is 20 months old, is the first baby in the UK to receive the life-saving gene therapy treatment Libmeldy for MLD. The treatment is now available for NHS patients after the health service managed to negotiate a significant and confidential reduction in the cost of it. However, it is still the most expensive drug licenced for use in Europe.
MLD is a deadly genetic disease which results in a life expectancy for children with it of just a few short years due to the severity of the damage it does to their nervous system and internal organs. The most common form of MLD usually develops in babies younger than 30 months and can lead to loss of sight, speech and hearing, as well as difficulty moving, brain impairment, seizures and eventually death in childhood.
Advertisement
Hide AdAdvertisement
Hide AdIt prevents the development of a crucial enzyme that leads to a build-up of fats that then destroy the protective layers around the child’s nerves. it is extremely rare, with only around four babies born in England each year estimated to have it.


The life-saving gene therapy works by removing the child’s stem cells and replacing the faulty gene that causes MLD before re-injecting the treated cells into the patient. Previously there was nothing hospitals and medical professionals could do beyond managing the symptoms and offering supportive care.
Teddi was the first person in the UK to receive the treatment outside of a clinical trial. The medical process began when she was 12 months old with the removal of stem cells at the end of June last year. These were then treated before the transplant took place in August. Teddi was discharged from the Royal Manchester Children’s Hospital (RMCH) back to her home in Northumberland in October.
Several months on from the procedure, Teddi has fully recovered from the transplant and is showing no signs of the devastating disease she was born with.
Advertisement
Hide AdAdvertisement
Hide AdTragically, though, Teddi’s three-year-old sister Nala also has MLD but her older sibling was not eligible for the treatment because the clinical guidance requires the gene treatment to be administered before the irreversible damage caused by the disease progresses too far. Both Teddi and Nala were diagnosed with the genetic disorder in April 2022.


The treatment is available to babies and young children with no clinical signs or symptoms, as well as those with early symptoms of the condition, so long as they can still walk independently and with no evidence of cognitive decline.
The treatment Teddi received is available on the NHS as a specialist service and is being delivered in Manchester by the RMCH in collaboration with the Manchester Centre for Genomic Medicine at Saint Mary’s Hospital. These are both part of the Manchester University NHS Foundation Trust (MFT).
The centre in Manchester is one of just five European sites administering the treatment, and the only one in the UK.
What has Teddi’s family said about the treatment?
Advertisement
Hide AdAdvertisement
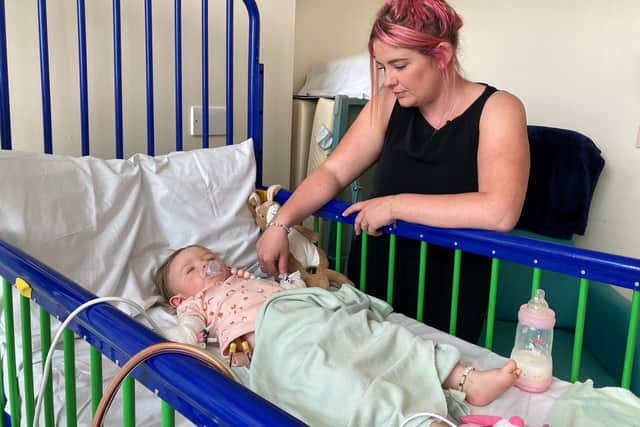
Hide AdTeddi and Nala’s mother Ally Shaw, 32, said: “In April last year, our world was turned upside down when not one, but both of our daughters were diagnosed with MLD. Being told our first daughter, Nala, wasn’t eligible for any treatment, would continue to lose all functions, and die extremely young was the most heart-breaking and hardest thing to come to terms with.
“However, amongst the pain, was hope for our younger daughter, Teddi. We were told that a new gene therapy treatment had, luckily, recently been made available on the NHS.
“We are extremely privileged that Teddi is the first child to receive this on the NHS and grateful that she has the opportunity to lead a long and hopefully normal life. Without this treatment, we would be facing both our children being taken away.

“We can only hope that one day, a treatment becomes available for all stages of MLD, and we feel strongly that it should be added to the newborn screening test to save more families from having to go through this heartache.
Advertisement
Hide AdAdvertisement
Hide Ad“We would like to say a huge thank you to our specialists, doctors and nurses and all the staff at Royal Manchester Children’s Hospital who have been fantastic in caring not just for Teddi, but us as a family.
“Teddi is doing absolutely brilliant! She is walking, running, a chatterbox, absolutely no signs so far of MLD. She is an absolute character and has everyone around her laughing all the time.”
What have the hospital and the medical experts said?
Professor Rob Wynn, consultant paediatric haematologist at RMCH and director of the hospital’s paediatric bone marrow transplant programme, said: “Being able to offer this first licenced treatment as part of NHS standard of care and, crucially, transform Teddi’s life, has been an exciting experience for all of us involved here in Manchester – staff, researchers, patients and families.
“Through the years, colleagues and I have looked after a range of patients with rare but severe conditions, where treatment has been limited. It is wonderful to be involved in this breakthrough moment and deliver a gene therapy which will transform outcomes for patients with MLD.
Advertisement
Hide AdAdvertisement
Hide Ad“It has been wonderful to care for Teddi and the Shaw family and our entire team wishes them well as she continues her recovery at home.”
Professor Simon Jones, consultant in paediatric inherited metabolic disease at the Manchester Centre for Genomic Medicine at Saint Mary’s Hospital and clinical director of the NIHR Manchester Clinical Research Facility at RMCH, said: “MLD is a progressive, life-limiting condition and, prior to this metabolic disorder service being made available via the NHS, there were no approved treatment options available.
“While there are various sub-types of the condition, in its later stages, all forms largely result in children losing their ability to move and speak. I care for many patients with later stage MLD and can testify to the devastating impact it can have.


“It is therefore enormously welcome that we are now able to offer Libmeldy treatment via the NHS, which is testament to the rigorous clinical trials that have paved the way for this decision, and the world-leading research and innovation capability within the UK healthcare system.
Advertisement
Hide AdAdvertisement
Hide Ad“As a trust, we are delighted to be selected as one of five European centres to deliver this new service as part of NHS standard of care, furthering our work as a European centre of excellence for metabolic conditions.”
NHS chief executive Amanda Pritchard said: “This is a huge moment of hope for parents and their babies who are born with this devastating inherited disorder, that can now be treated with a single round of revolutionary treatment at a specialist centre on the NHS.
“Thanks to advancements in gene therapies, and the commercial ability of the NHS to strike deals for cutting-edge drugs and then deliver them through our phenomenally skilled specialist staff, children born with this condition now have the opportunity to lead normal, healthy lives.
“It means that children like Teddi can do the things that all children should be able to, like going to school and playing with friends.
Advertisement
Hide AdAdvertisement
Hide Ad“I am delighted that we have given this miracle treatment to the Shaw family at what must have been a horrendous time for them, and I would like to thank the staff at Royal Manchester Children Hospital for turning research into reality for Teddi and others who will benefit.”
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.
